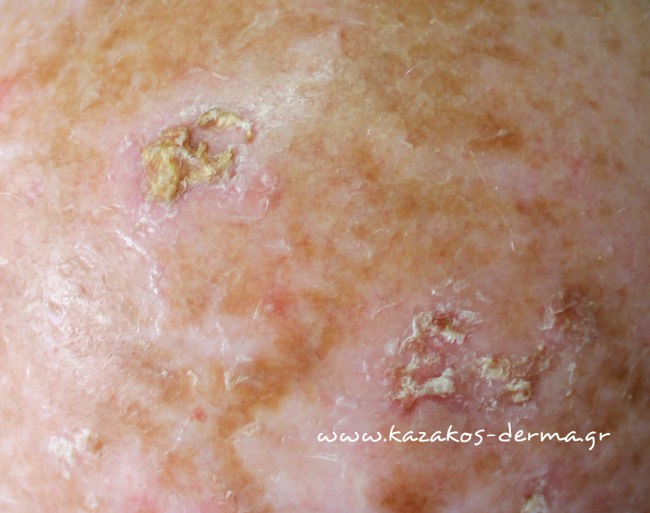
Actinic hyperkeratosis is a frequent reason for attendance in the dermatology clinic. These are red or brown plaques with a characteristic scaly appearance on their surface. The scaly surface can be thin or thicker. They are common in photoaged skin in older and younger patients. The most common sites of appearance of the lesions are on the face, scalp, earlobes, back, dorsal surfaces of the hands. They usually have no symptoms or sometimes have a mild itch.
-What causes the appearance of actinic hyperkeratosis?
The main cause of its appearance is the long-term unprotected exposure of the affected areas of the skin to ultraviolet radiation. Our skin is an organ with a long "memory" that manifests damage due to the cumulative and long-term harmful effects of the sun.
-Is actinic hyperkeratosis skin cancer?
Actinic hyperkeratosis at a pathological level is a highly differentiated squamous cell carcinoma that does not progress beyond the epidermis.
However, the term cancer is a strong one for a lesion that can remain for many years without worsening. Therefore, based on the clinical behavior of actinic keratosis, we prefer to consider it as προκαρκινική βλάβη.
Essentially, the appearance of such lesions is a warning bell for the patient. It means that the skin has now exhausted its resistance to ultraviolet radiation and needs protection, treatment and monitoring.
-How are actinic hyperkeratosis treated?
We usually treat actinic hyperkeratosis with conservative and invasive methods. However, the treatment plan is long. This is especially true if the lesions are numerous.
The main preservatives are
- Topical preparations with retinoids
- Topical application of diclofenac
- Topical application of immunomodulatory agents (imiquimod, ingenol mebutate, 5-FU)
- 5-ALA or M-ALA for photodynamic therapy using a special lamp or sunlight
Conservative treatment methods are extremely popular in "field treatments." That is, we apply them to areas that suffer heavily from multiple actinic hyperkeratosis.
The main invasive methods are
- Cryotherapy
- Dermabrasion
- CO2 laser cauterization2
- Cauterization with diathermocoagulation
With invasive methods we aim to destroy specific lesions.
Often a combination of invasive and conservative treatment methods is necessary to achieve a good result.
-How do we treat actinic hyperkeratosis with cryotherapy?
The cryotherapy is the most common invasive method of destroying such a lesion. The dermatologist applies liquid nitrogen to the lesion. The treatment is quick and does not require anesthesia. The feeling during application is a well-tolerated sting. Immediately after 24 hours, a dry scab appears in the area. It goes away on its own after a few days. The new skin is pink and needs sun protection.
We prefer to avoid cryotherapy during the summer months.
-How often does actinic hyperkeratosis recur?
Actinic hyperkeratosis is particularly "stubborn" and resistant to treatment. The reason is that it is very difficult to completely destroy all the epidermal cells mutated by ultraviolet radiation. For this reason, long treatment plans with many cauterization sessions and the use of topical treatments are necessary.
-How often does actinic hyperkeratosis develop into skin cancer?
The chance of an actinic hyperkeratosis changing into squamous cell skin cancer is small. However, areas with many and untreated lesions often develop skin cancer more frequently. Therefore, regular monitoring and treatment of these lesions is essential.
–Prophylactic agents for patients with actinic hyperkeratosis
Patients with actinic hyperkeratosis should use sun protection. It is recommended to use a sunscreen with a high protection factor (SPF>50). Also, those who work outdoors should use a hat and long-sleeved clothing.
Book your appointment with us immediately for any questions you may have!